A partnership involving Emory Healthcare, Royal Perth Hospital in Australia and health technology company Philips will move night intensive care work in the Emory eICU Center into daylight hours, focusing on the globalization of critical care medicine. The new project will allow Emory physicians and nurses to deliver care from the other side of the Earth by working in daylight hours in Australia to cover nighttime hours in Atlanta.
The vision to turn “night into day” was developed by Timothy Buchman, PhD, MD, founding director of the Emory Critical Care Center and Cheryl Hiddleson, MSN, RN, director of the Emory eICU Center.
“Emory is committed to the globalization of critical care and to partnerships that make this possible,” says Buchman. “Tele ICU medicine provides another option when a bedside intensivist is not available, because patients and providers benefit not only from having remote access to medical experts, these experts can also be available around-the-clock via an advanced bi-directional audio visual platform. We believe we can provide critical care to a patient no matter where they are in the world.”
By placing providers in a time zone with a 12-hour time difference, the providers come to work in Perth, Australia at 7am but cover the night shift remotely in Emory Healthcare ICUs beginning at 7pm. The time change transforms the experience for health care providers working at night, reversing two of the largest drawbacks of critical care night staffing: a shortage of senior clinicians willing to cover the night shifts and the toll that working nights takes on caregivers and their attention levels.
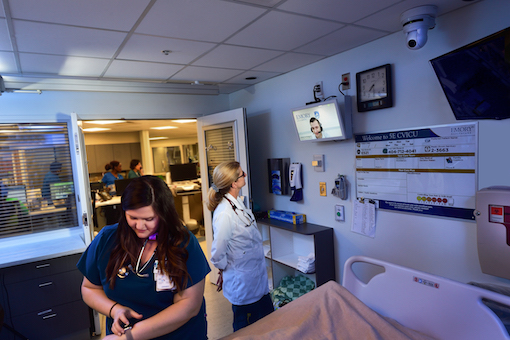
At Emory University Hospital, nurse Melissa Morris (left) works with a patient while nurse Lisa Walls speaks remotely with Milad Sharifpour, MD. Sharifpour, who is based in Perth, Australia, provides critical care services during daytime hours in Australia to cover nighttime hours in Emory's ICUs.
“In 2016, we initially tested the concept for six months during a trial or pilot project in Sydney, Australia and the benefits were immense, for both provider and patient,” says Buchman. “The providers worked more efficiently and felt better because they were working during daylight hours in Australia, reducing burnout and keeping more professionals satisfied in the critical care medicine field. Patients benefitted from the project by having focused, around-the-clock management of care, both during day and night hours.”
A specially-designed control room in Royal Perth Hospital is where the Emory providers work during daylight hours. Using remote electronic intensive care unit (eICU) technology by Philips, the providers can monitor the patient and speak directly to a care provider at the patient’s bedside in Atlanta, while also talking with the patient or family members. Specialized cameras, video monitors, microphones and speakers installed in Emory’s ICU rooms, at four of its hospitals and one non-Emory hospital, connect to the care team in Australia.
Importantly, the care teams at the bedside in Atlanta remain the primary caregivers. The providers in Australia work remotely to monitor patients and serve as back-up support in the event of emergency.
“Based on knowledge from our six-month pilot project, this new two- to three-year project in Perth will help us refine the eICU practice and the best delivery of care for our patients,” says Hiddleson. “Our goal is to optimize the remote practice in Perth with the correct number of care providers, the most effective duration of time spent on rotation along with other areas of focus to determine the best conditions for our providers caring for our patients back home.”
Currently, providers will spend eight to 16 weeks at a time on a rotation in Perth. Providers work in pairs with usually an intensivist physician and nurse teaming up in the control room for remote monitoring. And there has been no shortage of volunteers.

A specially-designed control room in Royal Perth Hospital is where Emory providers work during daylight hours in Australia to monitor critical care patients in Emory’s eICUs.
“Every clinician who has spent time in Australia on an eICU rotation wants to go back for additional rotations,” explains Hiddleson.
Emory Healthcare is no stranger to the eICU concept. In 2012, thanks to a $10.7 million Health Care Innovation Award from the Centers for Medicare and Medicaid Services (CMS), Emory launched an innovative plan to develop a collaborative network supporting intensive care units remotely throughout Georgia.
In 2014, the eICU program got underway in critical care units at Emory University Hospital, Emory University Hospital Midtown, Emory Saint Joseph’s Hospital, Emory Johns Creek Hospital and a small community hospital – East Georgia Regional Medical Center in Statesboro, Georgia. Health care workers were tasked with monitoring the five hospitals from a control room outfitted with equipment at Emory Saint Joseph’s Hospital. They provided continuous, 24/7 monitoring of critical care patients and access to intensivist physicians and other support staff on night and weekend shifts, when physicians were infrequently present in ICUs.
After three years in service, a report on the program determined the eICU program reduced length of patient stays in the ICU, resulted in fewer admissions, reduced costs by millions of dollars and helped solve the shortage of critical care intensivists. This eICU operation is still in use at Emory Healthcare today.
In addition to the collaboration with Emory across the globe, partners in Australia are hoping to expand the eICU concept to remote areas of that continent.
###
